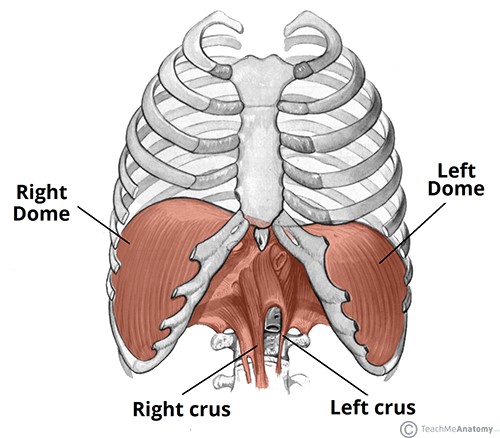
Inhale and exhale your pain away: the diaphragm muscle and how it relates to back pain!
August 31, 2015
What Is Pain and Why Do We Experience It Differently?
April 23, 2023Whether you’re preparing for a road/trail race, beginning a new training regimen, or simply aiming to increase your running load over the coming months, there are some important things to consider before doing so. A relatively common complaint among runners, both new and veteran, is knee pain. While there are many different reasons that this can occur, one is Patellofemoral Syndrome- or “Runner’s Knee” which refers to pain you may experience on the outer area of the knee.
Our DISC Sports Medicine Doctor, Dr. Djamel Senoussi, discusses this injury and how treatment and rehabilitation can help.
What is it?
Runner’s Knee or Patellofemoral Pain Syndrome (PFPS) or Patellofemoral Syndrome (PFS) refers to diffuse pain over the front of the knee, sometimes felt even on the back. Some of the causes can include activities that increase patellofemoral joint compressive forces (overload), such as squatting, ascending and descending stairs, and prolonged sitting, as well as repetitive activities such as running.
Why does this injury occur?
An imbalance between load and capacity of the body could be a factor leading to excessive load on the joint. This means: your body has a certain capacity to bear load, and going over that amount could lead to pain or injury.
There are a few variables to consider if you develop pain:
- LOAD: This simply refers to how much you are doing this activity. For this specific situation, we are referring to how much running you are doing, but can also be applied to other sports and training methodologies. (just think: load= how much you’re doing something)
Beginner runners
Beginner runners, or anyone starting up after an extended break; are in the adaptation process. Soft tissues start to react in order to allow the joint a suitable mobility pattern for running not only knees but also hips and ankles. The recovery capacity will also adapt to these changes.
Your body is adapting to something new so there are various ways your body will accommodate the increased strain.
Regular runners:
For athletes who run consistently, the adaptation process is already complete. Potential pain or injuries for this audience can occur after changes or adjustments are made to training or form. This includes changes in training intensity, duration, circuits, different shoes, or practicing other sports with a different requirement than running.
In addition to training variables, the following structural and physiological elements could play a role in injury. This is true for not only knee pain or running injuries but various other sports and training as well. We’ll refer to this as capacity.
- CAPACITY: Predisposing factors could be the source and sometimes the consequence
- Structural
This refers to any pre-existing conditions or issues that may contribute to additional pain or injury. Including:
– Malalignment (structural “patella baja, alta, trochlea dysplasia” or muscle imbalance)
-Mal traction (collateral soft tissues tightness, Hip internal rotation “anteversion of the femoral head”, excessive Q angle, Genu valgum, external tibial torsion, eversion of rearfoot)
-Quadriceps malfunction, Hip Abductors tightness, IT band stiffness
Chondromalacia (cartilage defects)
- Physiological
This refers to various lifestyle factors that could interfere with overall training and recovery. This includes, but is not limited to, sleep deficiency, additional stressors (work or home/family life), or anything that affects mental health and clarity.
What are some symptoms of PFS?
Pain anywhere around the kneecap even behind the knee triggered by the activity and sometimes present all the time
How is PFS Diagnosed?
It’s important to discuss patient history and symptoms. One of the most helpful ways to distinguish injuries or issues is to ask a series of questions to help guide us to an answer.
Typically, we will check for any predisposing conditions and the technical part of running (training intensity, duration, circuits, shoes), which are all of the elements listed above. From there, we can make a distinction between adaptation and impairment.
If more information is needed, we can use imaging to check the grade (severity) of some lesions.
How do you manage PFS?
Once diagnosed, physiotherapists can help manage the injury and restore a relative homeostasis load capacity (get you back to normal). They will also consider the amount of adaptation or changes needed to help prevent future issues. This can include:
- Combined work on the hip and knee, even ankles (homolateral/bilateral)
- Muscle activation and release of tensions
- Joint mobility: capsule, fascia, and ligament
Added to technical advice such as recovery tools and also a close follow-up while returning to activity and increasing load.
Happy training and happy running!
The post Knee Pain Explained: Runner’s Knee/PFS appeared first on Diversified Integrated Sports Clinic.
Source link